India is home to the largest number of children living with Type 1 Diabetes in the world. According to the IDF Diabetes Atlas 2025, over 301,000 Indian children are managing this lifelong autoimmune condition — often without a proper diagnosis, without affordable insulin, and without reliable information in a language that makes sense for their lives. Here you will learn about everything about type 1 diabetes in india
This guide is written for Indian families. Whether you are a parent who just heard the words “your child has Type 1 Diabetes,” a young adult managing injections through college hostels and Diwali dinners, or a caregiver trying to understand what this diagnosis really means — this is the most complete, medically accurate, and India-specific resource available.
We cover everything: what Type 1 Diabetes actually is, how it differs from Type 2, the early warning signs to catch before a crisis, how to manage insulin costs on an Indian budget, what to eat when your staple is roti and rice, and how to live fully — at school, at work, and at every festival.
What Is Type 1 Diabetes? Simple Explanation for Indian Readers
If you or your child has recently been diagnosed, the most important thing to understand is that Type 1 Diabetes is an autoimmune condition, not a lifestyle disease. In the simplest terms: your body’s defense system (the immune system), which is supposed to fight off germs, accidentally attacked the “insulin-producing factory” in your pancreas.
The “Lock and Key” Analogy: How Your Body Works
To understand Type 1, think of your body like a high-performance engine.
- The Fuel: Everything we eat—whether it’s a bowl of rice, a paratha, or a piece of fruit—is broken down into glucose (sugar). This glucose enters your blood and wants to get into your cells to give you energy.
- The Key (Insulin): Your pancreas produces a hormone called insulin. Think of insulin as a “Key.” Without this key, the door to your cells remains locked.
- The Problem: In Type 1 Diabetes, the body destroys the cells that make these keys. Because there are no “keys,” the sugar (glucose) stays trapped in your blood. This causes your blood sugar levels to skyrocket while your body’s cells are actually “starving” for energy.
Type 1 Diabetes in the Indian Context
India has the highest number of Type 1 Diabetes cases in the world. * Approximately 941,000 Indians are living with T1D.
- Over 301,000 of these are children and adolescents.
While the peak age for diagnosis is usually between 10 and 14 years old, the ADA 2026 Standards emphasize that Type 1 can actually develop at any age—even in adults. If you are part of this community, you are not alone; you are part of a massive, resilient network of nearly a million people.
Signs & Symptoms: The Warning Signals to Watch For
Symptoms of Type 1 often appear “out of the blue” over just a few weeks. Early recognition is a medical priority. If you notice these signs, consult a doctor immediately:
- The “Unquenchable” Thirst: Drinking liters of water but still feeling a dry mouth.
- Frequent Urination: Especially if a child starts wetting the bed again or needs to use the bathroom multiple times at night.
- Unexplained Weight Loss: Losing weight rapidly despite eating normally or even more than usual.
- Extreme Fatigue: Feeling “drained” and lacking the energy to play or work.
- Blurred Vision: High sugar levels can temporarily change the shape of the lens in your eye.
Medical Warning (DKA): If left untreated, the total lack of insulin leads to Diabetic Ketoacidosis (DKA). This is a severe emergency characterized by abdominal pain, vomiting, and a fruity smell on the breath. The 2024 ICMR guidelines stress that DKA requires immediate hospitalization.
Management: Living a Full Life with Insulin
Currently, there is no way to “cure” or “prevent” Type 1 through diet or herbs. Because the body can no longer make insulin, we must provide it from the outside.
- Lifelong Support: This means daily insulin via injections or an insulin pump.
- The Balancing Act: Managing T1D is about matching your insulin doses to the food you eat (especially Indian staples like rice or roti) and your physical activity.
Insulin isn’t “medicine”—it is a life-saving fuel. With the right education and modern technology like Continuous Glucose Monitors (CGM), a Type 1 diagnosis is no longer a limitation. It is a manageable condition that allows for a long, vibrant, and successful life.
Type 1 vs Type 2 Diabetes: Key Differences Every Indian Must Know
We cover it in a separate article in detail, lets discuss type 1 vs type 2 diabetes difference here in short
1. The Core Problem: Autoimmunity vs. Resistance
- Type 1 (The “Missing Key”): This is an autoimmune condition. For reasons not fully understood (likely a mix of genetics and environmental triggers), the body’s immune system mistakenly attacks the pancreas. The result? The body produces little to no insulin.
- Type 2 (The “Broken Lock”): This is primarily a condition of insulin resistance. The body still makes insulin (at least initially), but the cells don’t “respond” to it properly. Think of it as having the key, but the lock is jammed. Over time, the pancreas gets “tired” and its insulin production also starts to decline.
2. Causes & Prevention: Luck of the Draw vs. Lifestyle
- Type 1: There is currently no way to prevent Type 1. It is not caused by lifestyle choices, weight, or diet. It is linked to specific genetic markers and external triggers that researchers are still studying.
- Type 2: This is strongly influenced by lifestyle factors—such as being overweight and physical inactivity—alongside a strong genetic predisposition. According to the ICMR-NIN 2024 guidelines, Type 2 can often be prevented or delayed through a high-fiber, low-GI diet and regular exercise.
3. Age of Onset & Body Type
- Type 1: Historically called “Juvenile Diabetes” because it is most often diagnosed in children and adolescents (peaking around puberty). Individuals are typically lean and may experience sudden, dramatic weight loss right before diagnosis.
- Type 2: Traditionally seen in adults over 40, but in India, we are seeing a “metabolic shift” where it is increasingly diagnosed in younger adults and even children. People with Type 2 are usually overweight or obese at the time of onset.
4. Symptoms: The “Lightning Bolt” vs. The “Slow Burn”
- Type 1: Symptoms appear suddenly and severely—often over just a few weeks. About 25% of Type 1 cases in India are only discovered when a patient hits a life-threatening emergency called Diabetic Ketoacidosis (DKA).
- Type 2: Symptoms are often so mild and gradual that they go unnoticed for years. Many Indians only discover they have Type 2 during a routine health check-up or when a complication (like blurry vision or a slow-healing wound) arises.
5. Treatment: Survival vs. Management
- Type 1: Because the body produces zero insulin, people with Type 1 require lifelong, daily insulin (via injections or a pump) to survive. There is no alternative.
- Type 2: Management starts with lifestyle—Medical Nutrition Therapy (MNT) and exercise—and oral medications like Metformin. While some Type 2 patients eventually need insulin, it is not always required from Day 1.
6. Prevalence: The “Common” vs. The “Unique”
Type 2 is the “giant” of the diabetes world, accounting for more than 95% of cases globally and in India. However, because Type 1 is less common, it is often misunderstood, leading to social stigma.
In our Indian context, Type 2 is often unfairly called the “lazy person’s disease,” while Type 1 is treated with pity. Both are incorrect and harmful.
The ADA 2026 Standards emphasize Person-First Language. We don’t call someone a “diabetic”; we call them a “person living with diabetes.” This shift in language is crucial for our mission of education. Whether it is Type 1 or Type 2, the goal remains the same: mastering your blood sugar so you can live a life without limits.
How Common Is Type 1 Diabetes in India? The Reality Behind the Numbers
When we talk about the “Diabetes Capital of the World,” the conversation usually centers on lifestyle-related Type 2 diabetes. However, the data regarding Type 1 Diabetes (T1D) in India is even more striking—and for many, quite shocking.
I believe these numbers shouldn’t cause panic, but they should spark awareness. Understanding the scale of T1D in our country is the first step toward better diagnosis and saving lives.
India’s Global Standing: A Leader We Shouldn’t Be
According to the latest clinical registries and global health data, India is profoundly impacted by Type 1 diabetes, accounting for some of the highest prevalence statistics in the world.
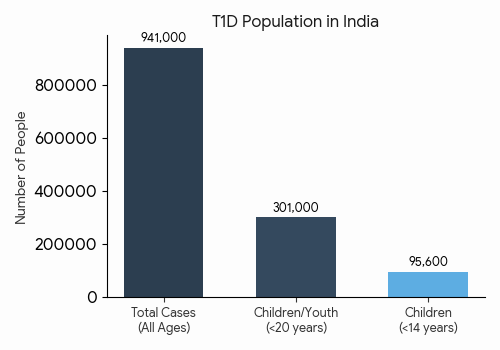
- The Total Impact: Currently, there are 941,000 people of all ages living with Type 1 diabetes in India. This puts us in the #2 spot globally, right behind the United States.
- The Youth Crisis: Most alarmingly, India ranks number one in the world for children and adolescents (under 20 years old) living with T1D, with an estimated 301,000 cases.
- The Growing Numbers: In children below 14 years of age, we see approximately 15,900 new cases diagnosed every single year.
When Does it Strike? The Age of Onset
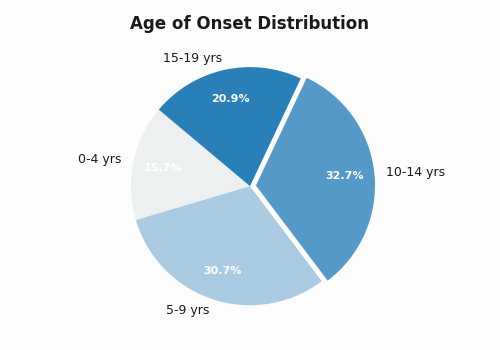
While you can develop Type 1 at any age, the data from the Registry of Youth Onset Diabetes in India (YDR) shows a very clear peak. The average age of onset in India is 10.5 years old.
Here is how the cases are distributed among our youth:
- Ages 0–4: 15.7% (Early childhood)
- Ages 5–9: 30.7% (Primary school years)
- Ages 10–14: 32.7% (The Peak Presentation)
- Ages 15–19: 20.9% (Late adolescence)
The Danger of Delayed Diagnosis: The DKA Statistic
Perhaps the most concerning statistic is this: 28.7% of Indian youth are already in Diabetic Ketoacidosis (DKA) by the time they are diagnosed. DKA is a life-threatening emergency where the blood becomes acidic due to a lack of insulin. In India, this happens far too often because T1D symptoms—like heavy breathing or abdominal pain—are frequently misdiagnosed as pneumonia or a stomach bug. Early recognition of the “4 Ts” (Thirst, Toilet, Tiredness, Thinner) is quite literally a matter of life and death.
The Unique Challenges of the “Indian Context”
Beyond the numbers, managing T1D in India involves hurdles that Western patients rarely face:
- The Cold Chain: In many parts of India, maintaining the “cold chain” (keeping insulin between 2°C and 8°C) is difficult due to power outages or lack of refrigeration.
- Affordability of Tech: While Continuous Glucose Monitors (CGMs) and insulin pumps are the gold standard in the ADA 2026 guidelines, they remain financially out of reach for many Indian families.
- The Complication Risk: Without consistent monitoring and expert care, our youth are at a high risk for early-onset complications like retinopathy (vision loss), nephropathy (kidney damage), and neuropathy.
What Causes Type 1 Diabetes? Myths vs. Medical Facts
When a family in India hears the word “Diabetes,” the first thought is usually about sugar, sweets, and lifestyle. But when it comes to Type 1 Diabetes (T1D), these thoughts are not just wrong—they are harmful. To manage T1D effectively, we must first clear the air. Type 1 is not a “lifestyle disease”; it is a complex biological event.
The Medical Fact: An Autoimmune “Glitch”
The primary cause of Type 1 diabetes is an autoimmune reaction. Think of your immune system as a specialized security team meant to protect you from viruses and bacteria. In T1D, this security team experiences a “glitch” and identifies your own insulin-producing beta cells in the pancreas as “foreign invaders.”
The immune system then launches an attack, destroying these cells. Once they are gone, the “insulin factory” closes down. While we don’t know the exact “on-switch” for this attack, science points to two main factors:
Genetic Susceptibility: You are born with a certain “blueprint.” Researchers have identified specific HLA genes (specifically DR3-DQ2 and DR4-DQ8) that are present in 30–40% of people with Type 1. However, genetics is not destiny. Even if one identical twin has T1D, there is only a 30% chance the other will get it.
Environmental Triggers: Since genes alone don’t cause T1D, something in the environment likely “triggers” the immune system. Current research (highlighted in the ADA 2026 Standards) suggests factors like enteroviral infections, rapid early-life weight gain, or even extreme stress on the beta cells may play a role.
Busting the Myths: What T1D is NOT
Because Type 2 is so common in India, people often apply T2D “rules” to Type 1. Let’s set the record straight:
- Myth: “Eating too much sugar or a poor lifestyle caused this.”
- The Fact: This is the most damaging myth in India. Sugar does NOT cause Type 1 diabetes. Unlike Type 2, which is linked to weight and activity levels, Type 1 is strictly an autoimmune and genetic condition. A child who eats zero sugar can still develop Type 1.
- Myth: “Only children get Type 1.”
- The Fact: While it was once called “juvenile diabetes,” we now know you can be diagnosed at any age. In fact, many Indian adults in their 30s or 40s are mistakenly told they have Type 2 when they actually have “Late-onset Type 1.”
- Myth: “It can be prevented if caught early.”
- The Fact: At this moment, there is no known way to prevent Type 1. While scientists are working on therapies to delay the onset, the underlying autoimmune attack cannot be stopped by diet, herbs, or lifestyle changes once it begins.
- Myth: “If it’s in the family, you will definitely get it.”
- The Fact: Actually, the vast majority of people diagnosed with Type 1 have no first-degree relatives with the condition. The risk is only about 3% if the mother has it and 5% if the father has it.
Early Warning Signs: The “4 Ts” Every Indian Parent Must Know
In Type 1 Diabetes (T1D), symptoms don’t just “drift” in—they often arrive like a storm. Because the body completely stops producing insulin, the onset is rapid. To protect your family, you must memorize the “4 Ts.” These are the red flags endorsed by the 2022 ICMR T1D Guidelines and the ADA.
- Toilet: Is your child visiting the bathroom more often, especially at night? Sudden bedwetting in a potty-trained child or unusually heavy diapers in infants are signs the kidneys are working overtime to flush out excess sugar.
- Thirsty: An extreme, “unquenchable” thirst. This isn’t just normal hydration; it’s a sign of severe dehydration as the body loses fluid through frequent urination.
- Tired: Constant sluggishness. Because sugar is trapped in the blood and cannot enter the cells for fuel, the body is literally “running on an empty tank.”
- Thinner: Rapid, unexplained weight loss. Starved for energy, the body begins breaking down its own fat and muscle for survival.
If you notice these signs, do not wait. A missed diagnosis can lead to Diabetic Ketoacidosis (DKA), a life-threatening emergency. Demand a simple finger-prick blood glucose test from your doctor immediately—it is the quickest way to rule out Type 1.
How Is Type 1 Diabetes Diagnosed in India? Tests & What They Cost.
Getting a diagnosis for Type 1 Diabetes (T1D) is often a whirlwind of emotions. For many Indian families, the journey begins in an emergency room, while for others, it’s a routine check-up after noticing the “4 Ts.”
According to the ICMR 2022 Guidelines and the ADA 2026 Standards, a diagnosis isn’t just about finding “high sugar”—it’s about proving that the body’s immune system has specifically targeted the pancreas.
The “First Responders”: Standard Blood Sugar Tests
To confirm that diabetes is present, your doctor will use one or more of these standard tests:
- Fasting Plasma Glucose (FPG): This is done first thing in the morning on an empty stomach.
- Random Plasma Glucose: This can be taken at any time. If the reading is 200mg/dl or higher and is accompanied by symptoms like extreme thirst or weight loss, it is a clear diagnostic signal.
- HbA1c (The 3-Month Report Card): This measures your average blood sugar over the last 90 days. A result of 6.5% or higher indicates diabetes.
- Oral Glucose Tolerance Test (OGTT): Often used when results are borderline, you drink a sugary liquid, and sugar is measured two hours later. A result of ≥ 200 mg/dL is diagnostic.
The “Tie-Breakers”: Specialized Type 1 Tests
In India, Type 2 diabetes is increasingly common in children, which can lead to confusion. To confirm it is definitely Type 1, doctors look for “Autoimmune Markers.”
- Autoantibody Tests: These look for specific proteins that prove the immune system is attacking the pancreas (GADA, ICA, etc.). These markers are found in 70–90% of people with T1D.
- C-Peptide Test: Think of this as checking the “smoke” to see if there is a “fire.” C-peptide is a byproduct of natural insulin. If your C-peptide levels are extremely low, it means your “insulin factory” has stopped working—a hallmark of Type 1.
- Ketone Testing: This is a survival check. When the body has zero insulin, it burns fat for fuel, creating “Ketones.” High levels lead to Diabetic Ketoacidosis (DKA). Shockingly, 28.7% of Indian youth are already in DKA by the time they are diagnosed.
The “Indian Challenge”: Avoiding Misdiagnosis
The ICMR warns that T1D symptoms in India are often mistaken for:
- Malaria or Typhoid
- Pneumonia
- Gastroenteritis (Stomach flu)
Furthermore, in states like Kerala and Tamil Nadu, doctors must differentiate T1D from Fibrocalculous Pancreatic Diabetes (FCPD), a unique regional form of diabetes. This is why specialized testing is non-negotiable.
Understanding the Financial Commitment (INR)
Managing Type 1 involves a significant financial shift. Based on the latest global health data (converted for our Indian context), here is the breakdown of what families can expect:
- Autoantibody Screening: A specialized screening panel for relatives of T1D patients (like those offered through international networks) costs approximately ₹1,150 to ₹1,200.
- The “First Year” Reality: Globally, the total burden of the first year of care—including hospital stays for DKA, purchasing insulin, and acquiring high-tech supplies—can average around ₹16.8 – 20 Lakhs.
While this number sounds daunting, the ADA 2026 Standards emphasize that early diagnosis prevents the most expensive part: ICU stays for DKA. In India, many government programs and NGOs are working to reduce these “out-of-pocket” costs for life-saving insulin.
Type 1 Diabetes Treatment in India: Insulin, Devices & Technology Overview
Living with Type 1 Diabetes (T1D) is essentially like taking over a job your pancreas used to do for free. Because your body no longer makes insulin, you have to become the “Chief Biological Officer” of your own health.
According to the 2022 ICMR Guidelines and 2026 ADA Standards, the goal is “Euglycemia”—keeping your blood sugar as close to a non-diabetic range as safely possible. Here is your roadmap to the tools and tech available in India today.
1. Mastering the Insulin Regimen
In India, we generally see two ways of replacing insulin. Think of this as choosing between a “Custom Suit” and “Ready-to-Wear.”
- The Gold Standard (Basal-Bolus / MDI): This is the “Custom Suit.” You take one long-acting injection (Basal) to cover your body’s background needs and one rapid-acting injection (Bolus) before every meal. This mimics a real pancreas and offers the most flexibility for Indian diets—whether you’re eating a light salad or a heavy festive thali.
- The Convenience Choice (Pre-Mixed): Often used in India to reduce the number of pricks. It combines two types of insulin in one shot. While simpler, it is less flexible; you must eat a specific amount of carbs at a specific time, which can be tough with unpredictable Indian meal timings.
2. The “Indian Summer” Storage Hack
One of the biggest hurdles in remote or rural India is the “Cold Chain.” Insulin must stay between 2°C and 8°C. If you don’t have a reliable fridge, the ICMR Guidelines offer a brilliant, time-tested solution:
- The Matka Hack: Store your insulin vials in a small earthen pitcher (Matka) filled with water. The natural evaporation keeps the insulin significantly cooler than the outside air. You can also use a wide-mouth thermos with ice cubes for travel.
3. Delivery Tools: Syringes vs. Pens vs. Pumps
- Syringes & Vials: The most affordable option. Crucial Safety Note: In India, we have two concentrations: 40 IU/ml (Red Cap) and 100 IU/ml (Orange Cap). Never mix them! Using a 40 IU syringe with a 100 IU vial can lead to a dangerous overdose.
- Insulin Pens: Much more discreet for school or office. “Smart Pens” are now arriving in India, which track your doses on your phone—no more “Did I take my shot?” anxiety.
- Insulin Pumps (CSII): These are wearable devices that deliver insulin 24/7 through a tiny tube. They are the closest we have to a natural pancreas, though they remain a premium choice in the Indian market.
4. Monitoring: The “End of Finger-Pricks”?
- SMBG (Finger-Pricks): The standard glucometer is still the backbone of Indian T1D care.
- CGM (The “Sensor”): Wearable sensors (like FreeStyle Libre or Dexcom) now allow you to see your sugar levels every minute on your smartphone. The 2026 ADA Standards now recommend CGMs for almost all Type 1 patients to prevent “silent” nighttime lows (hypoglycemia).
5. The Future: We Are Getting Closer to a “Cure”
As a strategist with 15 years in this field, I’ve never been more excited. The global research mentioned in the 2025 IDF Atlas and ADA 2026 is moving toward a needle-free future:
- Once-Weekly Insulin: Trials for Insulin Icodec and Efsitora show that we might soon move from 365 background shots a year to just 52.
- The “Artificial Pancreas” (AID): Systems that link a CGM and a Pump with an algorithm are already life-changing for many Indians, automatically stopping insulin if it predicts a drop.
- Cell Therapy: Groundbreaking stem-cell trials (like those from Vertex) are successfully “re-growing” insulin-producing cells in patients. We are moving from “managing” to “repairing.”
The Indian Diet & Type 1 Diabetes: What to Eat, Limit & Avoid
If you have Type 1 Diabetes, you’ve probably been told to “avoid all sugar.” But the truth is more nuanced. Because your body doesn’t produce insulin, your diet isn’t about restriction—it’s about matching. Every gram of carbohydrate you eat needs a corresponding “match” of insulin.
While there is no single “perfect” diet, the ICMR 2022 T1D Guidelines emphasize a balanced Indian plate that respects our culture while protecting our blood sugar.
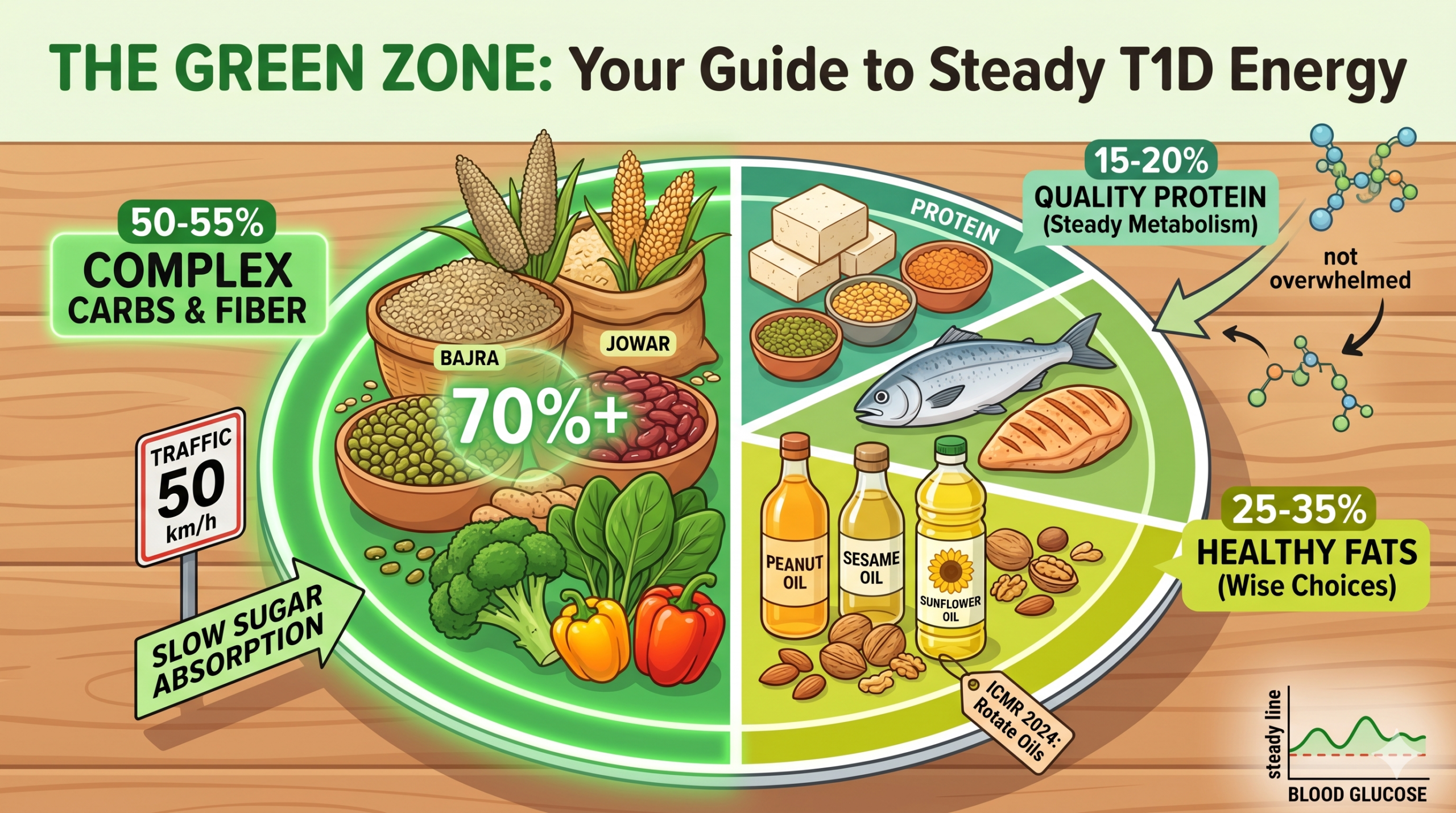
1. The “Green Zone”: What to Eat for Steady Energy
The goal is to choose “slow-release” fuels that don’t overwhelm your insulin.
- The 50% Rule for Complex Carbs: Carbohydrates should provide about 50–55% of your energy. The secret? High Fiber. At least 70% of your carbs should come from whole grains and millets (like Bajra or Jowar), legumes (Rajma, Moong, Chana), and fresh vegetables. Fiber acts like a “speed limit,” slowing down how fast sugar enters your blood.
- The Low-GI Heroes: Prioritize foods with a Low Glycemic Index. Excellent Indian staples include boiled Rajma, Moong Dal, and even Aged Basmati Rice. These give you a “slow burn” of energy rather than a sharp spike.
- Quality Protein (15-20%): Protein helps keep you full and stabilizes your metabolism. Mix vegetarian sources like Tofu and Dals with lean non-vegetarian options like fish or skinless chicken.
2. The “Yellow Zone”: What to Limit & Monitor
These aren’t “forbidden,” but they require expert-level insulin management.
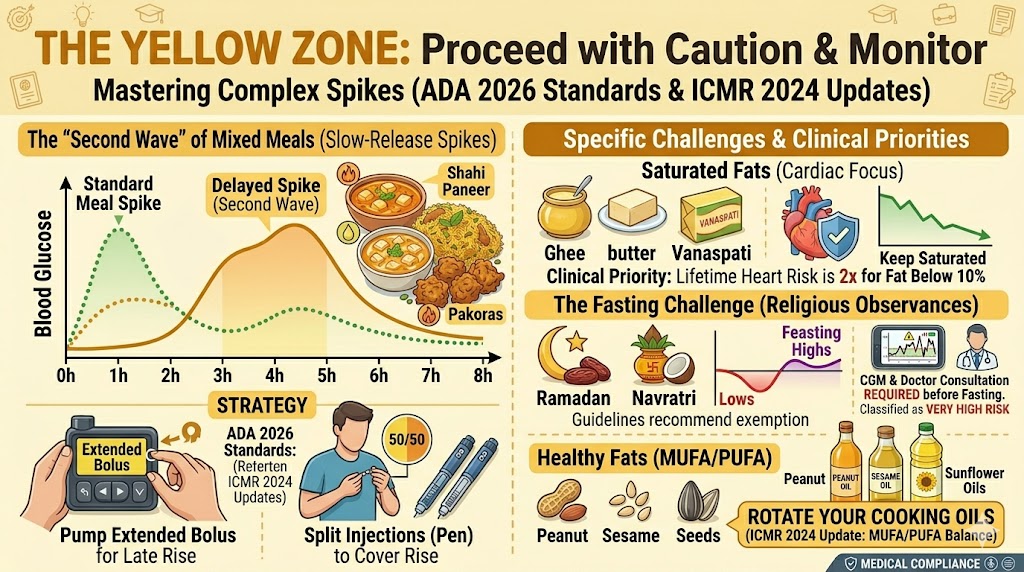

- The “Second Wave” (Mixed Meals): Rich Indian meals like Shahi Paneer, Biryani, or Pakoras are high in both fat and protein. These digest very slowly, causing a “delayed” sugar spike 3 to 5 hours after you’ve finished eating.
- The Strategy: To handle this “stubborn spike,” the ADA 2026 Standards suggest using an “Extended Bolus” on your pump or splitting your insulin injections to cover the late rise.
- Saturated Fats: Limit Ghee, butter, and Vanaspati. People with T1D have a higher lifetime risk of heart disease, so keeping saturated fat below 10% of your calories is a clinical priority.
- The Fasting Challenge: Religious fasts (Navratri, Ramadan) are classified as “Very High Risk” for T1D. The risk of life-threatening “lows” (hypoglycemia) followed by “feasting highs” is extreme. Most medical guidelines recommend exempting T1D individuals from strict fasting. If you choose to fast, you must use a CGM and consult your doctor for a specific insulin adjustment.
- Healthy Fats (25-35%): Don’t fear fat, but choose wisely. Use oils rich in MUFA/PUFA like peanut, sesame, or sunflower oil. TheICMR 2024 update suggests rotating your cooking oils to get a healthy balance of Omega-3 and Omega-6.
3. The “Red Zone”: What to Avoid for Better Control
These foods trigger “metabolic sprints” that are nearly impossible to match with insulin accurately.

- Liquid Sugar: Regular sodas, fruit juices, and sweetened lassi cause an almost instant spike. Water, buttermilk (Chaas), or infused water are your best friends.
- Simple Sugars: Table sugar (sucrose) should be less than 5% of your diet.
- Traditional Sweets: Jalebi, Rasmalai, and Gulab Jamun are “sugar bombs” that can send your blood sugar into the 300+ mg/dL range within minutes. If you have them, treat them as a rare, tiny portion paired with a fiber-rich meal.
Insulin Cost in India 2025-2026: What Families Actually Pay Per Month
For an Indian family, a Type 1 diagnosis is often followed by a terrifying question: “How much will this cost us every month?” Unlike Type 2, insulin is not a “choice”—it is the literal air a person with T1D breathes. In 2026, with no universal outpatient coverage under Ayushman Bharat, these costs fall squarely on your shoulders.
The Monthly Math: Branded vs. Biosimilar
According to the ADA 2026 Standards, the “Basal-Bolus” regimen is the gold standard. In India, your monthly bill depends entirely on the “Name” on the box:
- Branded Analogues (The Premium Choice): Using brands like Lantus or Novorapid via insulin pens typically costs between ₹4,000 and ₹5,000 per month.
- The “Smart Swap” (Biosimilars): Clinical research shows that biosimilars like Basalog (Biocon) or Basugine (Lupin) are medically equivalent to expensive brands but cost 15–20% less. This swap alone can save a family up to ₹6,000 per year.
India’s Best-Kept Secret: Jan Aushadhi Kendras
The biggest “insider tip” for Indian families is the Pradhan Mantri Bhartiya Jan Aushadhi Pariyojana (PMBJP). These government pharmacies provide high-quality generic insulin (Glargine and Regular) at 50–90% below market rates. By switching to Jan Aushadhi vials and syringes, a family can reduce their monthly insulin spend to under ₹1,000.
3 Ways to Slash Your Monthly Bill
- Locate a Kendra: Use the
pmbjpportal to find your nearest generic pharmacy. - Request Biosimilars: Ask your endocrinologist if Basalog is right for you. It’s the same molecule, just a smarter price.
- Check for Free Programs: The Changing Diabetes in Children (CDiC) program and NGOs like Blue Circle Diabetes Foundation often provide free or subsidized insulin for those under 18.
The Bottom Line: Managing T1D is a marathon. By using government schemes and biosimilars, you can provide world-class care for your loved one without breaking the bank.
Living Well with Type 1 Diabetes in India: School, Work & Festivals
Type 1 Diabetes isn’t a barrier; it’s a lifestyle adjustment. Whether it’s the school playground or a high-pressure office, the goal is to integrate T1D into your routine seamlessly.
The School “Care Network”
A child’s safety depends on an educated support system. According to the 2022 ICMR Guidelines, parents should inform teachers and bus drivers about the signs of hypoglycemia.
- The Survival Kit: Every school bag must contain a “safety kit” with glucose powder, biscuits, and a glucometer.
- Early Independence: We recommend fostering “micro-independence” early. Children aged 7+ should be encouraged to perform their own finger-pricks, building the confidence needed for a life without limits.
Workplace & Road Safety
For adults, transparency is your best safety net. Inform a trusted colleague where your emergency sugar is kept. Before hitting the Indian roads, follow the “Test Before You Trek” rule. Since even mild “lows” can impair your judgment, always keep non-perishable, low-GI snacks like roasted chana or peanuts in your vehicle.
Navigating Festivals & Fasting
India’s festivals are our cultural heart, but religious fasts (like Ramadan, Navratri, or Karwa Chauth) present extreme risks of DKA and dehydration. The IDF-DAR (Diabetes and Ramadan) guidelines classify T1D as “Very High Risk,” and medical exemptions are often recommended.
If you choose to fast, follow these clinical strategies:
- Insulin Tweak: Work with your doctor to reduce pre-dawn (Suhoor) insulin by 25–50% to avoid dangerous daytime “lows.”
- The Myth-Buster: Checking your blood sugar does not invalidate a religious fast. Monitor frequently, especially after the evening feast, and prioritize high-fiber, low-GI carbs to avoid the “feasting spike.”
By planning ahead, you don’t just “manage” the festivities—you participate in them with total metabolic confidence.
Mental Health & Diabetes Burnout: You Are Not Alone
Managing Type 1 Diabetes (T1D) is a 24/7 job with no vacations or sick leave. It is entirely normal—and medically expected—to feel exhausted. According to the ADA 2026 Standards of Care, the psychological toll of T1D is just as critical to treat as your HbA1c levels.
Distress vs. Burnout: The Emotional Toll
Nearly 50% of people living with T1D experience Diabetes Distress—the heavy feeling of defeat when blood sugars spike despite your best efforts. If left unaddressed, this can lead to Diabetes Burnout, where emotional exhaustion causes you to stop checking sugars or missing doses. In India, where mental health is often stigmatized, many suffer in silence.
The Vicious Cycle of Stress and Sugar
Mental health and biology are a two-way street. When you are stressed, your body releases cortisol, a hormone that acts like a “sugar tap,” causing blood glucose to rise. This creates a frustrating cycle: stress causes high sugar, and high sugar causes more stress and irritability.
Strategies for Resilience
You can break the cycle of burnout with these science-backed steps:
- Set “SMART” Goals: Stop chasing perfection. Focus on small, achievable wins, like checking your sugar three times a day.
- Leverage Technology: The ADA 2026 guidelines highlight that CGMs (Sensors) and Insulin Pumps drastically reduce the “cognitive burden” of T1D by doing the mental math for you.
- Find Your Tribe: Peer support is life-saving. Connect with Indian communities like the Blue Circle Diabetes Foundation to share the “daily grind” with those who truly understand.
My advice: Your mind deserves as much care as your pancreas. If you feel overwhelmed, seek integrated care where your psychologist and endocrinologist work together.
Finding the Right Doctor for Type 1 Diabetes in India
In India, finding a Type 1 Diabetes (T1D) specialist can sometimes feel like searching for a needle in a haystack, especially if you live outside a major city. While many doctors are experts in Type 2, Type 1 requires a very specific, high-tech, and personalized approach.
The most important thing to know is that you don’t just need one doctor—you need a “Diabetes Dream Team.”
Your T1D Support Squad
According to the ICMR 2022 Guidelines, managing T1D is a team sport. To stay healthy, look for these key players:
- The Captain (Endocrinologist): A specialist in hormones who understands the “math” of insulin. They set your doses and guide your overall care.
- The Coach (Diabetes Educator): They teach you the “survival skills”—how to prick your finger, give injections properly, and handle “sick days.”
- The Guide (Dietitian): Since Indian food is naturally high in carbs, you need an expert to help you count carbs for your specific meals like Poha, Roti, or Idli.
- The Support (Psychologist): Managing T1D 24/7 is exhausting. A counselor helps you fight “Diabetes Burnout” and stay mentally strong.
How to Find Expert Care Anywhere in India
If you live in a remote area or a small town, technology is now closing the gap:
- Use Telemedicine: You can now consult top T1D experts in cities like Delhi, Mumbai, or Bangalore via your smartphone. This is a game-changer for regular check-ups.
- Join the Community: Connect with the Blue Circle Diabetes Foundation. They are India’s largest patient-led community. Their mobile app and helplines are the best way to find trusted local doctor recommendations from people who are walking in your shoes.
- Search for “Pediatric Endocrinologists”: If your child is diagnosed, this specific search term will lead you to doctors who specialize in young people with Type 1.
My Advice: If your current treatment (like tablets) isn’t working, or if your doctor doesn’t mention CGMs or Insulin Pumps, it may be time for a second opinion from a T1D specialist.
FAQ
Can Type 1 Diabetes be cured in India?
No cure exists; it requires lifelong insulin
What is the difference between Type 1 and Type 2 diabetes?
Type 1 is an autoimmune lack of insulin; Type 2 involves insulin resistance
for details refer this article T1D vs T2D
Can a child with Type 1 Diabetes live a normal life in India?
Yes, with daily management and support to the patient. Go to better pediatric endocrinologist, purchase medicines from pmbjp government generic medical stores.
Is insulin available for free in India?
No, but some charities provide financial aid. you can also buy effective generic insulin medicines.
What foods should a Type 1 diabetic avoid in India?
Avoid sugary drinks, packaged foods, and high-sugar sweets. Understand the glycemic index and go for low GI foods.
How much does Type 1 Diabetes management cost per month in India?
Monthly costs vary, but first-year care averages $20,000 globally.
About the author
It’s me Mohammad Junaid Rain an MBBS student at GMC Nagpur, passionate about making evidence-based medical information accessible to every Indian. “medstuffs.com” is dedicated to clear, doctor-written disease education for patients and caregivers.
Disclaimer: This article is for educational purposes only and does not substitute professional medical advice. Please consult your doctor for diagnosis and treatment.

2 thoughts on “Type 1 Diabetes in India: The Complete 2026 Guide — Symptoms, Diet, Insulin & Living Well”