Diabetes is like a lock on your body’s door. Insulin is the key. But in type 2 diabetes, the key stops working properly. Exercise doesn’t just help, it actually fixes the lock. That’s why Exercise Routine for Type 2 Diabetes is very essential.
When someone is newly diagnosed with type 2 diabetes, the very first thing doctors recommend is not always a tablet. It’s movement. Exercise, along with a good diet, is the foundation of diabetes treatment worldwide. It’s not optional, its medical treatment.
You dont need months to see a difference. Research shows that just 7 days of regular exercise can improve how your body handles blood sugar, even without losing a single kilogram of weight. Your body starts responding almost immediately.
HbA1c is the 3-month blood sugar report card your doctor checks.
Studies show that people who exercised regularly for 20 weeks had significantly better HbA1c than those who didn’t. And the harder they exercised, the better the improvement.
In simple terms — exercise improves the very test your doctor uses to judge your diabetes control.
When you exercise, your body doesn’t just burn calories. It repairs 4 important organs that diabetes damages:
| Organ | What Exercise Does |
|---|---|
| Muscles | Absorbs sugar from blood directly |
| Liver | Stops making extra sugar unnecessarily |
| Fat cells | Reduces harmful inflammation |
| Pancreas | Helps it produce insulin better |
No single medicine does all four at once. Exercise does.
Here’s the honest truth — exercise benefits start fading after just 48 to 96 hours of stopping.
This means if you exercise Monday and then skip Tuesday and Wednesday — your body is already losing the benefit by Thursday.
This is why consistency beats intensity. A 30-minute walk every day is far better than a 2-hour gym session once a week.
In our pharmacology classes, we learn that Metformin works by reducing the liver’s excess sugar production. Interestingly, exercise does the exact same thing — completely naturally, with zero side effects.
How Exercise Lowers Blood Sugar
Have you ever wondered what actually happens inside your body when you go for a walk after dinner? Your blood sugar drops — but how?
When you exercise, your muscles need energy fast. So they start pulling sugar directly from your blood — without even needing insulin. This is the key point most people miss.
In normal diabetes treatment, insulin acts like a delivery boy — carrying sugar from blood into cells. But exercise creates a shortcut. It activates a special protein called GLUT4 inside your muscle cells that opens a direct door for sugar to enter — no insulin required.
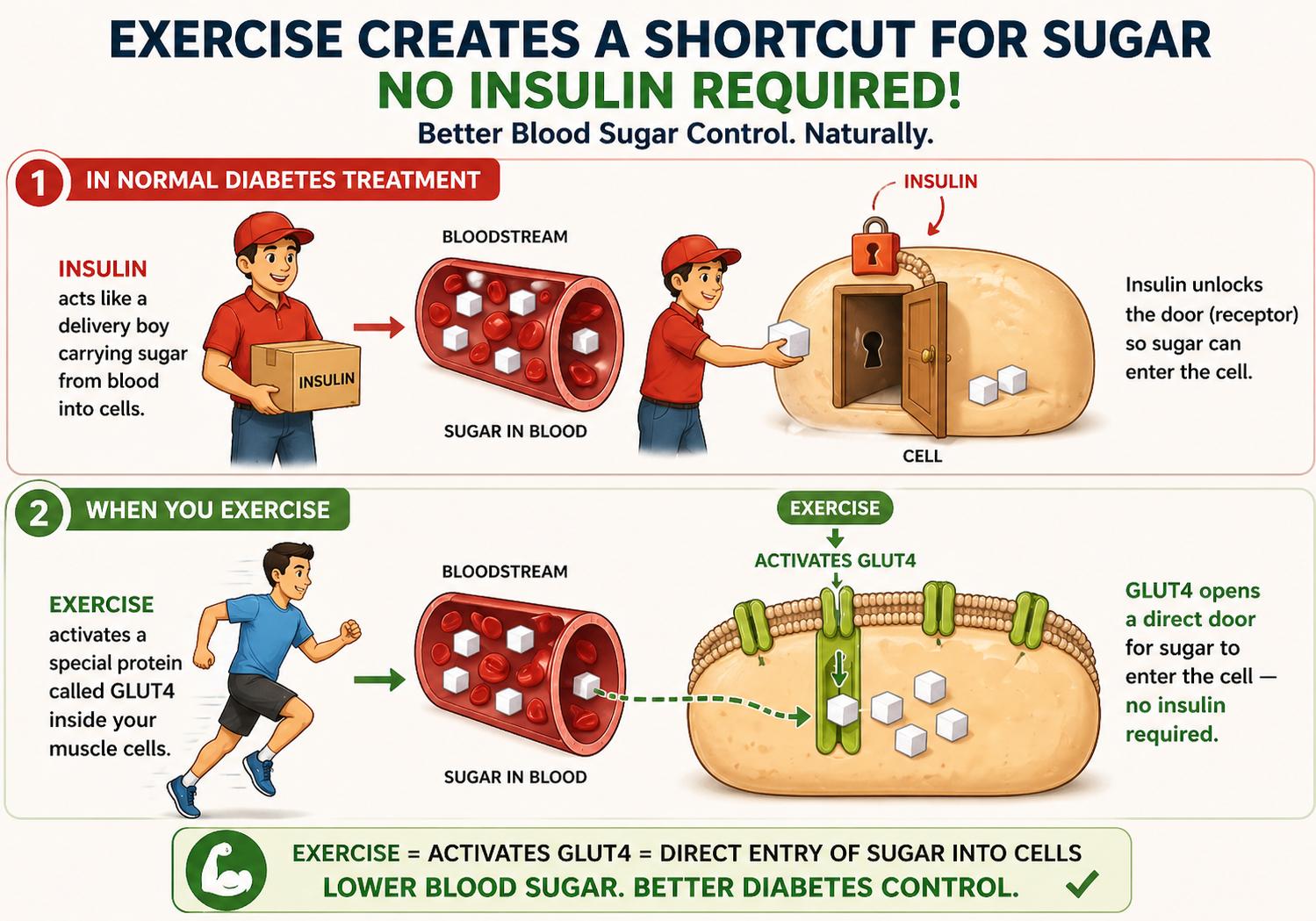
Think of it like this — insulin is the key to the door. Exercise breaks the door open entirely.
A Note From The Author “In our pharmacology and physiology classes as MBBS students, we study exactly how insulin signals glucose uptake in skeletal muscle. What surprised me when I first learned this — exercise activates the same glucose transport pathway as insulin, but through a completely separate route. This means even when insulin resistance is high, exercise can still work. That’s why doctors call it the most underused prescription in diabetes management.” — Mohammad Junaid Rain, MBBS 2nd Year
According to a study published in the American Physiological Society, just 2 weeks of regular exercise significantly increased GLUT4 protein levels in muscles, improved blood sugar control, and enhanced mitochondrial function in Type 2 diabetic patients.
Additionally, research from PMC — The Essential Role of Exercise in T2D confirms that a single bout of exercise can temporarily increase muscle sugar absorption by up to 5 times compared to rest.
Even better — this blood sugar lowering effect continues for 24 to 72 hours after you stop exercising.
This means your evening walk today is still protecting you tomorrow morning.
The bottom line — exercise lowers blood sugar both immediately and for days after. No pill does that.
Aerobic Exercise: Types, Duration, Frequency
Think of aerobic exercise as your blood sugar’s best friend.
When you move your large muscles rhythmically — walking, cycling, swimming — your body pulls glucose out of the bloodstream for energy. The result? Your blood sugar drops naturally, without medication.
How much should you do?
The American Diabetes Association recommends at least 150 minutes of moderate-to-vigorous aerobic activity every week, spread across a minimum of 3 days — with no more than 2 consecutive days of rest in between.
That works out to just 30 minutes a day, 5 days a week. Completely doable.
What counts as aerobic exercise?
You have plenty of options — pick what you enjoy:
| Exercise | Intensity Level | Best For |
|---|---|---|
| Brisk walking | Moderate | Beginners |
| Cycling (outdoor/stationary) | Moderate | Joint-friendly option |
| Swimming | Moderate–Vigorous | Those with neuropathy or joint pain |
| Dancing | Moderate | Fun + sustainable |
| Jogging / Running | Vigorous | Intermediate to advanced |
| Aerobics class | Moderate–Vigorous | Group motivation |
Strength Training: Why It Matters for Insulin Sensitivity
Most people with Type 2 diabetes focus only on walking or cardio. That’s a good start, but if you’re skipping strength training, you’re leaving one of the most powerful blood sugar tools on the table.
Here’s why it matters so much.
Muscle is your body’s glucose storage unit.
When you build muscle through resistance training, your body creates more “storage space” for blood sugar. More muscle = more places glucose can go, without needing insulin to get there. This is called improved insulin sensitivity, and it’s exactly what people with Type 2 diabetes need.
What does the research actually show?
The numbers are striking. A landmark ACSM + ADA joint study found that just twice-weekly progressive resistance training over 16 weeks produced:
| Outcome | Result |
|---|---|
| Insulin action improvement | +46.3% |
| Fasting blood glucose reduction | −7.1% |
| Visceral fat (belly fat) | Significant reduction |
These are meaningful, real-world results — from just two sessions per week.
What counts as strength training?
You don’t need a gym membership or heavy weights to start. Options include:
- Bodyweight exercises — squats, wall push-ups, lunges (perfect for beginners)
- Resistance bands — affordable, joint-friendly, easy to use at home
- Free weights or dumbbells — for progressive overload as you get stronger
- Weight machines — great for guided form if you go to a gym
How often should you train?
Aim for 2 to 3 sessions per week, targeting all major muscle groups — legs, back, chest, arms, and core. Allow at least one rest day between sessions so your muscles recover properly.
4-Week Beginner Workout Plan
Starting an exercise routine can feel overwhelming — especially if you haven’t been active in a while. This plan takes the guesswork out of it completely.
It’s designed for absolute beginners. No gym required. No equipment needed for the first two weeks.
The plan is built on what the ADA 2025 Standards actually recommend:
At least 150 minutes of moderate-to-vigorous aerobic activity per week, spread over a minimum of 3 days — plus 2 to 3 resistance training sessions per week on nonconsecutive days.
This plan delivers exactly that — gradually and safely.
🗓️ Week 1 — Just Get Moving (Low Intensity)
Goal: Build the habit. Don’t worry about intensity yet.
| Day | Activity | Duration |
|---|---|---|
| Monday | Brisk walk | 20 min |
| Tuesday | Bodyweight squats + wall push-ups (2 sets × 10 reps) | 15 min |
| Wednesday | Brisk walk | 20 min |
| Thursday | REST or gentle stretching | — |
| Friday | Brisk walk | 20 min |
| Saturday | Bodyweight squats + seated leg raises (2 sets × 10 reps) | 15 min |
| Sunday | REST | — |
Weekly aerobic total: ~60 min | Strength sessions: 2
🗓️ Week 2 — Build Consistency (Moderate Intensity)
Goal: Increase walk duration. Add one more strength move.
| Day | Activity | Duration |
|---|---|---|
| Monday | Brisk walk | 25 min |
| Tuesday | Squats + push-ups + resistance band rows (2 sets × 12 reps) | 20 min |
| Wednesday | Brisk walk | 25 min |
| Thursday | REST or light yoga | — |
| Friday | Brisk walk | 25 min |
| Saturday | Squats + lunges + shoulder press with bands (2 sets × 12 reps) | 20 min |
| Sunday | REST | — |
Weekly aerobic total: ~75 min | Strength sessions: 2
🗓️ Week 3 — Add Intensity (Moderate–Vigorous)
Goal: Hit 120+ aerobic minutes. Increase resistance sets.
| Day | Activity | Duration |
|---|---|---|
| Monday | Brisk walk + 5 min light jog intervals | 30 min |
| Tuesday | Strength circuit: squats, lunges, push-ups, band rows (3 sets × 12 reps) | 25 min |
| Wednesday | Brisk walk | 30 min |
| Thursday | REST | — |
| Friday | Brisk walk + 5 min jog intervals | 30 min |
| Saturday | Strength circuit (3 sets × 12–15 reps) | 25 min |
| Sunday | REST or 20-min easy walk | — |
Weekly aerobic total: ~120 min | Strength sessions: 2–3
🗓️ Week 4 — Hit the ADA Target (Full Routine)
Goal: Reach 150 aerobic minutes. Three strength sessions. Full ADA compliance.
| Day | Activity | Duration |
|---|---|---|
| Monday | Brisk walk / cycling | 30 min |
| Tuesday | Strength: full body circuit (3 sets × 15 reps) | 30 min |
| Wednesday | Brisk walk / swimming | 30 min |
| Thursday | Strength: upper body focus (3 sets × 15 reps) | 30 min |
| Friday | Brisk walk / jogging | 30 min |
| Saturday | Strength: lower body + core (3 sets × 15 reps) | 30 min |
| Sunday | REST | — |
Weekly aerobic total: 150 min ✅ | Strength sessions: 3 ✅
A few important rules before you begin:
- ✅ Always check your blood sugar before and after exercise (see the next section)
- ✅ Start slowly — some movement every day beats one intense session per week
- ✅ Stay hydrated throughout
- ✅ If you feel dizzy, chest pain, or extreme fatigue — stop and rest immediately
- ✅ Talk to your doctor before starting if you have any complications
Safety Tips: Exercising with High/Low Blood Sugar
Exercise is powerful medicine for Type 2 diabetes — but doing it safely matters just as much as doing it consistently.
Before you lace up your shoes, there’s one thing you need to understand: exercise affects your blood sugar in both directions. It can lower it too much, or sometimes push it temporarily higher. Knowing what to watch for keeps you safe and confident every time you work out.
Before You Start — Do You Need a Doctor’s Clearance?
Not always. Pre-exercise medical clearance is not necessary for asymptomatic, sedentary individuals who wish to begin low- or moderate-intensity physical activity not exceeding the demands of brisk walking.
However, if you have existing complications — heart disease, kidney disease, or neuropathy — always check with your doctor first.
What Is Hypoglycemia During Exercise?
Hypoglycemia means your blood sugar drops too low — typically below 70 mg/dL (3.9 mmol/L).
This can happen during or even several hours after exercise, especially if you take insulin or certain diabetes medications like sulfonylureas.
Warning signs to watch for:
- Sudden shakiness or trembling
- Sweating more than expected
- Dizziness or lightheadedness
- Rapid heartbeat
- Confusion or difficulty concentrating
- Feeling unusually weak mid-workout
What to do if it happens:
Stop exercising immediately. Follow the 15-15 rule:
- Take 15 grams of fast-acting carbohydrates — 4 glucose tablets, half a cup of fruit juice, or 3–4 teaspoons of sugar dissolved in water
- Wait 15 minutes, then recheck your blood sugar
- If still below 70 mg/dL, repeat once more
- Once stable, have a small snack before resuming activity
When Should You Delay Exercise?
If your blood sugar is too HIGH before exercise:
Starting intense exercise when blood sugar is already elevated can push it even higher in some cases, particularly with vigorous activity.
| Blood Sugar Level | What to Do |
|---|---|
| Below 90 mg/dL | Have a small carb snack before starting |
| 90–250 mg/dL | Safe to exercise — ideal range |
| Above 250 mg/dL | Proceed with caution; check for ketones if on insulin |
| Above 300 mg/dL | Delay exercise; consult your doctor |
Neuropathy & Special Precautions
If you have autonomic neuropathy (nerve damage affecting body functions), exercise requires extra care. Autonomic neuropathy may complicate exercise — precautions include avoiding rapid directional changes if orthostatic hypotension is present, and preventing dehydration during exercise with adequate fluid intake.
In simple terms:
- Rise slowly from lying or sitting positions before starting exercise
- Drink water before, during, and after every session
- Avoid sudden stops or direction changes if you feel dizzy or lightheaded
General Safety Rules for Every Workout
- ✅ Check blood sugar before and after every session
- ✅ Wear proper footwear — never exercise barefoot if you have neuropathy or foot complications
- ✅ Exercise with a buddy or in a public place when possible — especially as a beginner
- ✅ Carry your medical ID or diabetes alert card
- ✅ Keep your glucometer and fast-acting carbs nearby at all times
- ✅ Stay hydrated — dehydration can affect blood sugar readings and heart rate
- ✅ Cool down for 5 minutes after every session — stopping abruptly can cause blood pressure drops
Medical Disclaimer: The information in this section is for general educational purposes only. Always consult your doctor or diabetes care team before starting a new exercise program, especially if you take insulin or diabetes medications.
Best Exercises if You Have Complications (Neuropathy etc.)
Having diabetes complications doesn’t mean you stop exercising. In most cases, it means you exercise smarter — choosing activities that protect your body while still delivering real blood sugar benefits. Here’s what the evidence says for each major complication.
Diabetic Peripheral Neuropathy (Nerve Damage in Feet & Legs)
Neuropathy causes numbness, tingling, or pain — usually in the feet and lower legs. Many people with neuropathy avoid exercise fearing injury. But research shows the opposite approach works better.
Exercise training shows meaningful benefits for neuropathic symptoms and functional capacity in patients with diabetic peripheral neuropathy. The key is choosing low-impact, joint-friendly activities that don’t put excessive pressure on damaged nerves.
Best exercises for neuropathy:
| Exercise | Why It Works | Special Notes |
|---|---|---|
| Swimming & water aerobics | Zero ground impact, full-body movement | Excellent for severe foot numbness |
| Stationary cycling | No balance demands, low foot stress | Adjust seat height carefully |
| Seated resistance exercises | Builds muscle without standing stress | Bands and light weights work well |
| Tai chi | Improves balance and coordination | Reduces fall risk significantly |
| Chair yoga | Gentle stretching, flexibility, circulation | Good for beginners or elderly patients |
What to avoid with neuropathy:
- High-impact running or jumping (risk of undetected foot injury)
- Barefoot exercise of any kind
- Activities on uneven surfaces (fall risk due to balance issues)
💡 Foot check rule: Always inspect both feet before and after every workout. Because neuropathy reduces sensation, small cuts or blisters can go unnoticed and become serious infections if untreated.
Diabetic Retinopathy (Eye Damage)
If you have moderate to severe retinopathy, some types of exercise can temporarily raise pressure inside the eye — which may worsen the condition.
Avoid:
- Heavy weight lifting with straining or breath-holding (Valsalva maneuver)
- High-intensity interval training (HIIT) with extreme exertion
- Inverted positions (headstands, certain yoga poses)
Safe options:
- Brisk walking
- Light to moderate cycling
- Swimming at a comfortable pace
- Low-resistance strength training with controlled breathing
Always get clearance from your ophthalmologist before starting any new routine if you have active or proliferative retinopathy.
Diabetic Cardiovascular Complications
People with diabetes have a significantly elevated risk of heart disease. This doesn’t eliminate exercise — it makes it more important. But intensity needs to match your current cardiovascular fitness.
Safe starting points:
- Begin with 10–15 minute walks and build up gradually
- Monitor your heart rate — stay within 50–70% of your maximum heart rate for moderate intensity
- Avoid exercising in extreme heat or cold, which stresses the cardiovascular system
- Stop immediately and seek medical help if you experience chest pain, pressure, or sudden breathlessness
Balance & Fall Prevention — Often Overlooked
Neuropathy combined with poor muscle strength dramatically increases fall risk. Adding balance training to your routine is one of the most protective things you can do.
Simple balance exercises (no equipment needed):
- Single-leg stand — hold for 10–30 seconds each side (hold a chair for support initially)
- Heel-to-toe walking in a straight line
- Seated ankle circles and calf raises
- Standing side leg raises
Even 5–10 minutes of balance work three times a week can reduce fall risk meaningfully.
Medical Disclaimer: If you have any diabetes-related complications, always consult your doctor, endocrinologist, or physiotherapist before starting or modifying your exercise routine. This content is for educational purposes only and does not replace personalised medical advice.
FAQ :
Unsuitable exercise for type 2 diabetes
Some exercises can increase injury risk, joint stress, foot problems, or unsafe blood sugar fluctuations in people with Type 2 Diabetes, especially if complications are present.
Sprinting
Jumping workouts
Long-distance running on hard surfaces
Heavy weightlifting
Boxing
Martial arts sparring
Barefoot jogging
High-intensity workouts in extreme heat
Marathon training without planning
Strenuous inverted yoga poses
Exercise for type 2 diabetes at home
Regular home exercise can improve insulin sensitivity, lower blood sugar, support weight control, and help manage Type 2 Diabetes safely and consistently.
Brisk walking in place
Marching indoors
Chair squats
Wall push-ups
Sit-to-stand from chair
Step-ups on stairs
etc.
how does exercise help type 2 diabetes
Exercise helps Type 2 Diabetes by moving sugar from blood into muscles for energy and improving insulin sensitivity. It lowers post-meal blood sugar, reduces belly fat, supports weight loss, builds muscle, improves heart health, lowers stress, improves sleep, and can reduce HbA1c when done regularly and consistently.
Reference
1) https://pmc.ncbi.nlm.nih.gov/articles/PMC12167735/
2) https://www.ncbi.nlm.nih.gov/books/NBK549946/
3) https://diabetes.org/health-wellness/fitness/weekly-exercise-targets
4) Latest advances and controversies of exercise therapy in the management of type 2 diabetes
5) The essential role of exercise in the management of type 2 diabetes
About the author
Mohammad Junaid Rain is a 2nd-year MBBS student focused on simplifying diabetes care for Indian families. He creates evidence-based health content using medical textbooks, ADA guidance, ICMR resources, research papers, and clinical exposure. His goal is to make diabetes management practical and easy to understand for Indians.

