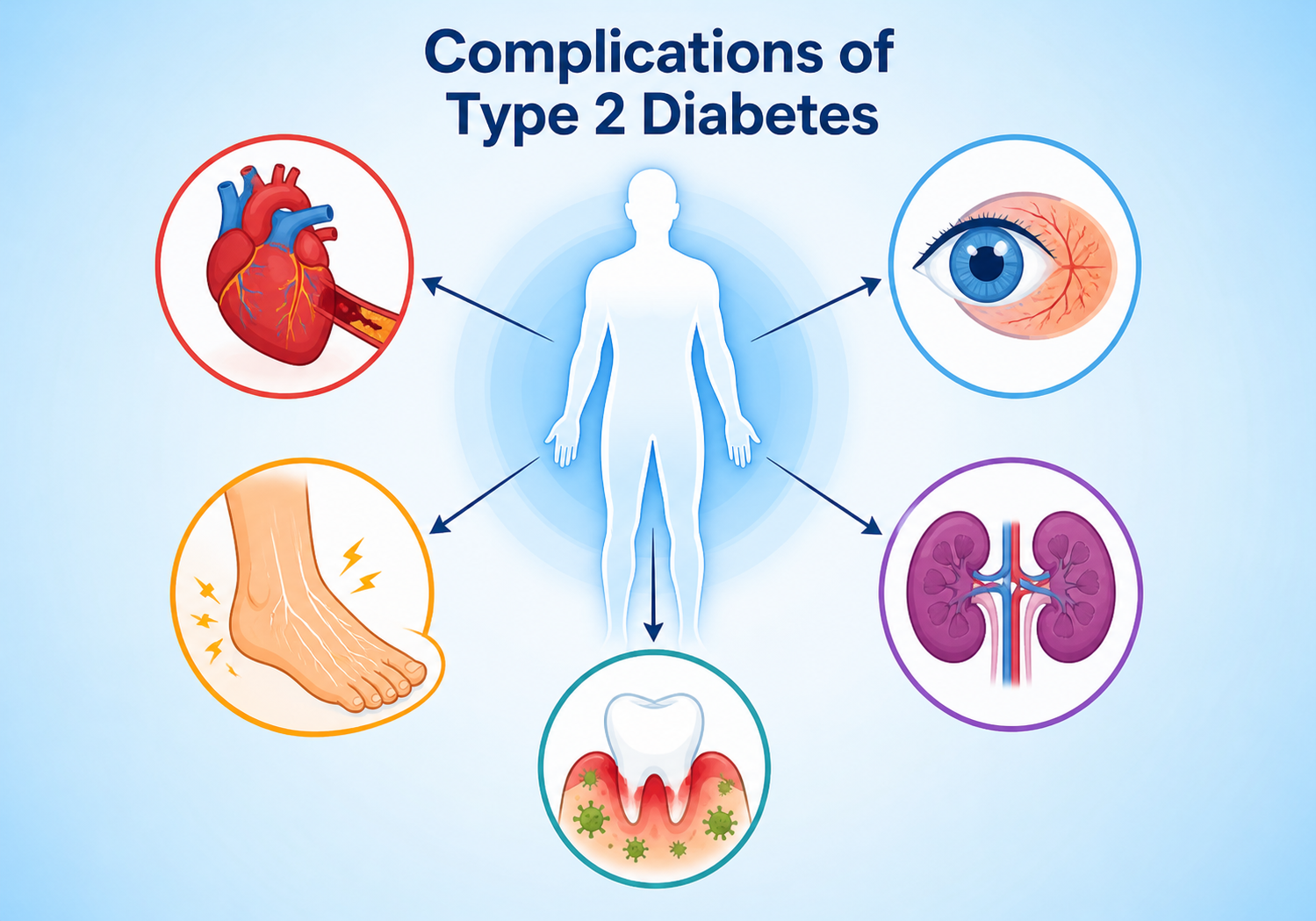
Every Indian family knows someone with diabetes. But very few know what happens inside the body when diabetes goes uncontrolled for years. Lets now learn about the complications of type 2 diabetes.
The truth is — Type 2 diabetes doesn’t just affect your blood sugar. Left unmanaged, it silently damages your heart, kidneys, eyes, nerves and feet — often before you even feel any symptoms.
In India, where 101 million people live with diabetes, complications are the real silent crisis. Thousands lose their eyesight, undergo kidney dialysis, or face limb amputation every year — not because treatment wasn’t available, but because they didn’t know what was coming.
This guide covers every major type 2 diabetes complication — what causes it, how to recognise early warning signs, and most importantly — how to prevent it.
Because prevention always beats treatment.
Why Uncontrolled Blood Sugar Damages the Body
You’ve heard doctors say — “Control your sugar.” But what actually happens when you don’t?
Here’s the answer — and it starts with your blood vessels.
Your body has millions of tiny blood vessels — called capillaries — that carry oxygen and nutrients to every organ. Your heart, kidneys, eyes, nerves and feet all depend on these vessels to stay alive and healthy.
When blood sugar stays high for months or years, it acts like slow-moving acid on these vessels.
It damages their inner walls. It makes them stiff, leaky and narrow. Blood flow reduces. Organs start getting less oxygen and fewer nutrients. And slowly — silently — they begin to fail.
Doctors call this process diabetic microangiopathy — damage to the small blood vessels. It is the root cause behind nearly every major diabetes complication.
From My Medical Studies “In our pathology classes, we study exactly how chronic hyperglycemia damages blood vessels. Excess glucose reacts with proteins in vessel walls through a process called glycation — forming harmful compounds called AGEs (Advanced Glycation End-products). These AGEs stiffen blood vessel walls, trigger inflammation, and slowly destroy the delicate lining of capillaries. What shocked me when I first learned this — the damage starts silently, years before any symptom appears. By the time a patient feels something is wrong, significant organ damage has often already occurred. This is why regular monitoring even without symptoms is not optional — it is essential.” — Mohammad Junaid Rain, MBBS 2nd Year.
According to WHO, diabetes leads over time to damage of the heart, blood vessels, eyes, kidneys and nerves — making it one of the most destructive chronic diseases globally when left uncontrolled.
High blood sugar damages the body through 4 main pathways:
| Pathway | What It Does | Organs Affected |
|---|---|---|
| AGE formation | Stiffens and destroys vessel walls | Eyes, kidneys, nerves |
| Oxidative stress | Creates free radicals that inflame vessels | Heart, blood vessels |
| Polyol pathway | Causes cells to swell and malfunction | Nerves, lens of eye |
| Inflammation | Triggers silent chronic damage | All organs |
The most dangerous part — none of these processes cause pain in the early stages.
This is why Type 2 diabetes is called a silent destroyer. The damage accumulates quietly for years — until one day a person is told they have kidney failure, or they are going blind, or their foot needs amputation.
The only protection is early detection, regular monitoring and consistent blood sugar control.
According to the landmark UKPDS (UK Prospective Diabetes Study), every 1% reduction in HbA1c reduces the risk of diabetes complications by up to 37%. That means controlling your sugar today is directly preventing organ damage tomorrow.
Reference:
Pathophysiology of Type 2 Diabetes Mellitus — PMC
The Pathobiology of Diabetic Complications — Diabetes Journal
Diabetes — WHO Fact Sheet 2024
Heart Disease & Stroke — The #1 Complication of Type 2 Diabetes
If there’s one complication of type 2 diabetes that deserves your full attention, it’s this one.
Nearly 52% of all deaths in people with type 2 diabetes are caused by heart disease. That’s not a small statistic — that’s the leading cause of death in this population, according to a major clinical review published in the World Journal of Diabetes.
Why Does Diabetes Hurt Your Heart?
Persistently high blood sugar slowly damages your blood vessels from the inside. Over time it triggers inflammation, makes your arteries stiff and narrow, and speeds up the buildup of fatty plaques — a process called atherosclerosis. The result? A heart that has to work harder through increasingly damaged pipelines.
The famous Framingham Heart Study found that diabetes raises the risk of heart attack 2 to 4 times — and heart failure risk by 4 to 6 times.
It’s Not Just Heart Attacks
Most people know diabetes raises heart attack risk. But the same review identifies two other cardiac complications that are far less talked about:
Cardiac Autonomic Neuropathy (CAN) — nerve damage that disrupts your heart’s rhythm and blood pressure control. It affects at least 20% of people with diabetes and often goes completely undetected.
Diabetic Cardiomyopathy (DCM) — where high blood sugar directly weakens the heart muscle itself, even without blocked arteries. Early signs of this are found in up to 75% of people with type 2 diabetes.
Your HbA1c Directly Affects Your Heart Risk
| HbA1c Level | Cardiovascular Death Risk |
|---|---|
| Below 6.9% | 2x higher than non-diabetics |
| 7.9% – 8.7% | 4x higher |
| Above 9.7% | 5x higher |
Every point of improvement in your HbA1c genuinely protects your heart.
The Good News
Heart disease in diabetes is largely preventable. Statins, newer diabetes medications like GLP-1 agonists and SGLT-2 inhibitors, blood pressure control, and weight loss have all been proven to significantly reduce cardiovascular risk.
Reference:
https://pmc.ncbi.nlm.nih.gov/articles/PMC8040078
Diabetic Kidney Disease (Nephropathy) — When Sugar Slowly Destroys Your Kidneys
Your kidneys are among the hardest working organs in your body.
Every single day they filter 200 litres of blood — removing waste, balancing fluids, and keeping your body clean from inside.
But here is the problem — your kidneys do this filtering through millions of tiny blood vessels. And as we learned earlier — high blood sugar destroys tiny blood vessels.
This means your kidneys are under direct attack every single day that blood sugar remains uncontrolled.
Over time this damage leads to a condition called Diabetic Nephropathy — or diabetic kidney disease.
How It Progresses — The Silent Stages
The frightening reality of diabetic kidney disease is how silently it develops:
| Stage | What’s Happening | Symptom |
|---|---|---|
| Early | Kidneys leaking small protein (microalbuminuria) | None — completely silent |
| Middle | Protein leakage increases, BP rises | Mild swelling, fatigue |
| Late | Kidney function declining significantly | Swelling, nausea, weakness |
| End stage | Kidney failure — dialysis needed | Severe symptoms |
Most Indian patients discover kidney damage only at the middle or late stage — because the early stage has absolutely no symptoms.
🩺 From My Medical Studies “In our medicine lectures, diabetic nephropathy is described as the leading cause of end-stage renal disease worldwide. What our professors emphasise repeatedly — the earliest detectable sign is microalbuminuria — a tiny amount of protein leaking into urine. This test costs less than ₹100 at any pathology lab. Yet most Indian diabetic patients have never had it done. Catching nephropathy at the microalbuminuria stage can literally save a patient’s kidneys — because at that point, the damage is still reversible with proper treatment.” — Mohammad Junaid Rain, MBBS 2nd Year
Key Warning Signs to Watch
- Swelling in feet and ankles — especially in evenings
- Foamy or frothy urine — sign of protein leakage
- Rising blood pressure despite medication
- Unexplained fatigue and weakness
- Reduced urine output in advanced stages
How to Protect Your Kidneys
According to PMC Diabetic Nephropathy Review 2023, the most effective kidney protection strategies are:
- Keep HbA1c below 7% consistently
- Keep blood pressure below 130/80 mmHg
- Take ACE inhibitors or ARBs if prescribed — they specifically protect kidney filters
- Avoid painkiller overuse — NSAIDs like Ibuprofen damage kidneys silently
- Get urine microalbumin test done every year — without fail
💡 Indian Specific Warning: In India, self-medication with painkillers like Ibuprofen, Diclofenac and Combiflam is extremely common. For diabetic patients — this is dangerous. These drugs reduce blood flow to already-stressed kidneys and can accelerate kidney failure significantly.
Reference:
Comprehensive Advancements in Prevention & Treatment of Diabetic Nephropathy — PMC 2023
New Strategies to Improve Clinical Outcomes for Diabetic Kidney Disease — PMC
Diabetic Nephropathy: Challenges in Pathogenesis, Diagnosis and Treatment — PMC
Eye damage (retinopathy) — leading cause of blindness
Imagine waking up one morning and noticing your vision is blurry.
You think — “Maybe I need new glasses.”
But your eye doctor tells you something far more serious — diabetes has been damaging your eyes for years. Silently. Without a single warning.
This is the reality of diabetic retinopathy — and it is the leading cause of blindness in adults aged 20–74 years worldwide.
In India, where millions of diabetics go years without an eye check-up, this complication is particularly devastating.
What is the Retina and Why Does It Matter?
Think of your eye like a camera.
The retina is the camera film at the back of your eye. It captures everything you see and sends signals to your brain.
Now imagine someone slowly pouring water into that camera — damaging the film from inside.
That is exactly what uncontrolled blood sugar does to your retina.
High blood sugar damages the tiny blood vessels supplying the retina. These vessels start leaking fluid and blood. New abnormal vessels grow. The retina gets damaged. Vision deteriorates.
And the most frightening part — you feel nothing until significant damage has already occurred.
The 4 Stages of Diabetic Retinopathy
| Stage | What’s Happening | Vision Impact |
|---|---|---|
| Mild NPDR | Small balloon-like swellings in vessels | No symptoms |
| Moderate NPDR | More vessels blocked | Mild blurring possible |
| Severe NPDR | Many vessels blocked, retina signals for new growth | Noticeable vision changes |
| PDR (Proliferative) | Abnormal new vessels grow and bleed | Severe vision loss or blindness |
NPDR = Non-Proliferative Diabetic Retinopathy PDR = Proliferative Diabetic Retinopathy — the most dangerous stage
From My Medical Studies “In our ophthalmology postings, we learned that diabetic retinopathy follows a predictable progression — from microaneurysms to haemorrhages to neovascularisation. What struck me most during clinical rounds was meeting patients who had perfect vision just 2 years ago — now facing permanent blindness — simply because they never got a dilated eye examination done. The tragedy is that early-stage retinopathy is completely treatable with laser therapy. But once the retina detaches or bleeds extensively — that vision cannot be restored. Prevention and early detection are the only weapons we have.” — Mohammad Junaid Rain, MBBS 2nd Year
Who is at Highest Risk?
According to ADA Standards of Care 2024, diabetic retinopathy risk increases significantly with:
- Diabetes duration above 10 years
- Consistently poor HbA1c control
- High blood pressure alongside diabetes
- Pregnancy with pre-existing diabetes
- Smoking — which damages blood vessels further
Warning Signs — Never Ignore These
| Symptom | What It May Mean |
|---|---|
| Sudden blurry vision | Fluid leaking into macula |
| Seeing floating spots or strings | Bleeding inside eye |
| Dark or empty areas in vision | Retinal damage |
| Difficulty seeing at night | Advanced retinopathy |
| Sudden vision loss | Emergency — go to doctor immediately |
⚠️ Critical Warning: Any sudden change in vision in a diabetic patient is a medical emergency. Do not wait for your next routine appointment. Go to an ophthalmologist immediately.
How to Protect Your Eyes
The PMC Retinopathy Prevention Guidelines recommend:
- Annual dilated eye examination — every diabetic patient, every year without fail
- Keep HbA1c below 7% — this single step reduces retinopathy risk by up to 76%
- Control blood pressure below 130/80 mmHg
- Stop smoking completely
- If retinopathy is detected early — laser photocoagulation can prevent progression
💡 Indian Specific Point: A dilated eye examination costs ₹200–500 at most government hospitals and ₹500–1500 at private eye clinics. Many Indians avoid it thinking their vision is fine. But retinopathy causes NO symptoms until it is advanced. Every diabetic patient must get this test done annually — regardless of how good their vision feels.
Can Diabetic Retinopathy Be Reversed?
Honest answer — early stages can be stabilised and progression stopped. Advanced stages cannot be fully reversed.
This is why the window of early detection is everything.
Laser treatment, anti-VEGF injections like Ranibizumab and Bevacizumab, and vitreoretinal surgery are available options — but they work best when retinopathy is caught early.
Reference:
ADA Standards of Care 2024: Retinopathy, Neuropathy & Foot Care — PMC
The Prevention and Treatment of Retinal Complications in Diabetes — PMC
Current Treatments and Innovations in Diabetic Retinopathy — PMC
Nerve Damage (Neuropathy) — Pain, Numbness and Digestive Issues
Have you ever heard a diabetic patient say —
“Mere paon mein bahut jalan hoti hai raat ko” — my feet burn terribly at night.
Or — “Mujhe pata hi nahi tha ki pair mein chot lag gayi” — I didn’t even know my foot was injured.
Both are classic signs of diabetic neuropathy — nerve damage caused by years of uncontrolled blood sugar.
According to AAFP 2024, diabetic peripheral neuropathy affects up to 50% of all diabetic patients — making it the most common complication of diabetes.
How High Blood Sugar Damages Nerves
Your nerves need a constant, steady blood supply to function. When tiny blood vessels supplying the nerves get damaged by high glucose — nerves slowly stop working properly.
Think of it like a wire losing its insulation. First it sparks — causing pain and burning. Then it goes completely dead — causing numbness where you feel nothing at all.
From My Medical Studies “In our neurology lectures, we study diabetic neuropathy as a length-dependent axonal degeneration — meaning the longest nerves in the body are damaged first. That is why symptoms always begin in the feet and toes before spreading upward — never the other way around. This pattern is so characteristic that when a patient describes burning feet that started at the toes and moved upward, diabetic neuropathy immediately comes to mind clinically. What concerns us as future doctors is that by the time a patient feels symptoms, significant nerve damage has already occurred.” — Mohammad Junaid Rain, MBBS 2nd Year
3 Types of Neuropathy Every Diabetic Must Know
1. Peripheral Neuropathy — Most Common Affects feet, legs and hands. Symptoms — burning pain, tingling, electric shock sensations, numbness, loss of sensation.
2. Autonomic Neuropathy — The Hidden One Affects internal organs — heart, stomach, bladder. Symptoms — bloating after meals, unpredictable loose motions or constipation, dizziness on standing, bladder problems.
💡 Indian Note: Many Indian diabetics complain of gas, bloating and irregular digestion for years without realising it is actually autonomic neuropathy — nerve damage affecting the stomach. This is called gastroparesis — where stomach emptying slows down significantly.
3. Focal Neuropathy — Sudden and Painful Affects a single specific nerve suddenly. Symptoms — sudden severe pain in thigh, wrist or eye muscle weakness.
How to Prevent Nerve Damage
- Keep HbA1c below 7% consistently — this is the single most effective prevention
- Check vitamin B12 levels yearly — especially if on Metformin long term
- Avoid alcohol completely — it directly damages nerves
- Daily foot inspection — look for cuts you cannot feel
- Report burning or tingling feet to your doctor early — do not dismiss it
Reference:
Diabetic Peripheral Neuropathy: Prevention and Treatment — AAFP 2024
Prevention and Management Strategies for Diabetic Neuropathy — PMC
Update on Management of Diabetic Neuropathy — PMC
Diabetic Foot — Wounds, Infections and Amputation Risk
Here is a story that happens in Indian hospitals every single day.
A diabetic patient comes to casualty. His family says — “Doctor, bas ek choti si chot thi joote se” — it was just a small shoe bite.
But the wound never healed. It got infected. It spread to the bone. And now the surgeon is discussing amputation.
This is diabetic foot — and it is entirely preventable.
Why Diabetic Feet Are So Vulnerable
Three things combine to make diabetic feet dangerously fragile:
1. No sensation — Neuropathy means you cannot feel pain. A stone in your shoe, a blister, a small cut — you feel nothing. The wound grows without your knowledge.
2. Poor blood supply — Damaged blood vessels mean wounds receive less oxygen and fewer healing nutrients. A cut that would heal in 5 days in a normal person takes weeks or never heals in a diabetic patient.
3. Weakened immunity — High blood sugar feeds bacteria. Infections spread faster and deeper in diabetic tissue than in anyone else.
According to PMC 2025, diabetes is the leading cause of non-traumatic lower limb amputation worldwide — and most amputations are preceded by a small, ignored wound.
From My Medical Studies “In our surgery postings, diabetic foot cases are heartbreakingly common. What our surgical faculty emphasises — the Wagner grading system classifies diabetic foot from Grade 0 (no wound, high risk) to Grade 5 (gangrene of entire foot). Most patients arrive at Grade 3 or 4 — deep infection reaching bone — when a simple Grade 0 screening and proper footwear could have prevented everything. Prevention costs nothing. Amputation costs everything.” — Mohammad Junaid Rain, MBBS 2nd Year
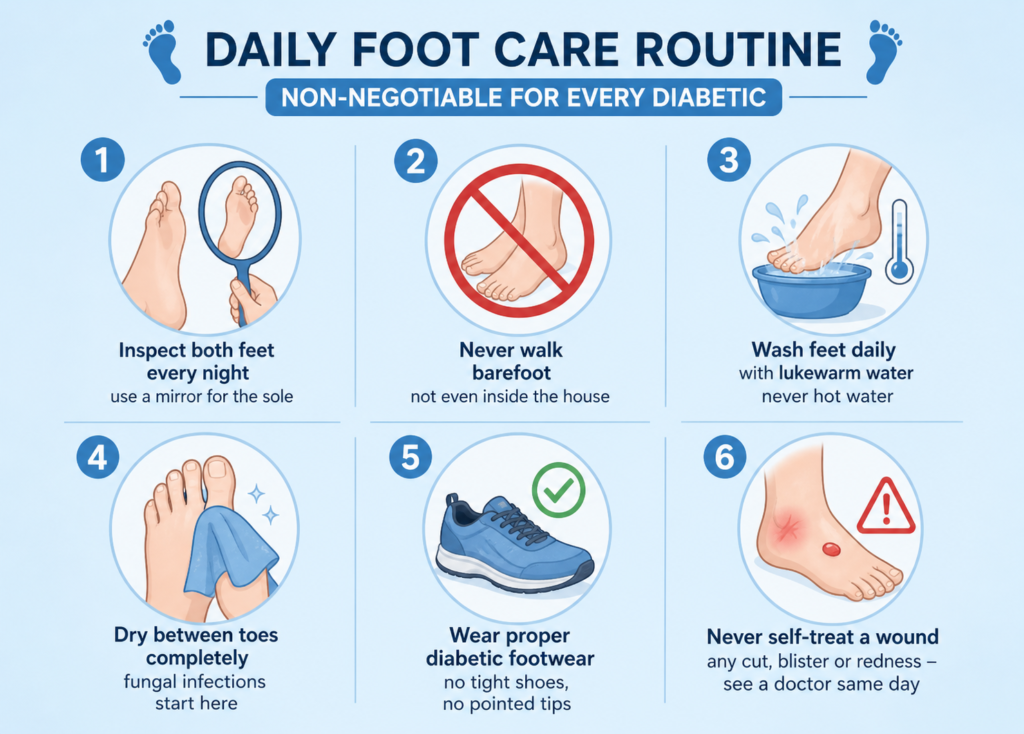
Daily Foot Care Routine — Non-Negotiable for Every Diabetic
- Inspect both feet every night — use a mirror for the sole
- Never walk barefoot — not even inside the house
- Wash feet daily with lukewarm water — never hot water
- Dry between toes completely — fungal infections start here
- Wear proper diabetic footwear — no tight shoes, no pointed tips
- Never self-treat a wound — any cut, blister or redness — see a doctor same day
⚠️ Indian Warning: Walking barefoot during pooja, in fields, or on hot summer roads is extremely common in India. For diabetic patients — this is one of the most dangerous habits. A single unnoticed injury on a numb foot can start a chain of events leading to amputation.
Reference:
Comprehensive Review on Diabetic Foot Ulcers — PMC 2025
Choice of Wound Care in Diabetic Foot Ulcer — PMC
ADA Standards of Care 2024 — Foot Care
Mental Health: Depression & Diabetes Distress — The Complication Nobody Talks About
When we talk about diabetes complications — everyone mentions kidneys, eyes, heart and feet.
But there is one complication that silently affects 1 in 3 Indian diabetic patients — and almost nobody discusses it.
Depression and diabetes distress.
Living with diabetes is exhausting. Every meal is a calculation. Every blood sugar reading brings anxiety. Every doctor visit brings fear. Every family gathering becomes a negotiation between enjoyment and discipline.
Over months and years — this mental burden becomes its own medical condition.
The Dangerous Two-Way Relationship
Diabetes and depression don’t just coexist — they make each other worse.
| Direction | What Happens |
|---|---|
| Diabetes → Depression | Chronic illness, lifestyle restrictions and complications cause persistent sadness and hopelessness |
| Depression → Diabetes | Depression reduces motivation to exercise, eat well and take medicines — blood sugar worsens |
According to PMC research, people with Type 2 diabetes have 2 times higher risk of developing depression compared to people without diabetes.
And depressed diabetic patients have significantly worse HbA1c, more complications and higher mortality.
This is not a weakness. This is a medical reality.
🩺 From My Medical Studies “In our psychiatry postings, our faculty introduced us to a term called ‘diabetes distress’ — which is different from clinical depression. Diabetes distress is the specific emotional burden of managing a lifelong condition — the fear of complications, the guilt of a bad meal, the exhaustion of constant self-monitoring. Studies show diabetes distress affects nearly 36% of people with Type 2 diabetes — yet it is almost never screened for in Indian OPDs. As future doctors, we are taught that treating the mind is as important as treating the blood sugar. A patient who is mentally broken cannot manage their diabetes effectively — no matter how good their prescription is.” — Mohammad Junaid Rain, MBBS 2nd Year
Warning Signs of Diabetes-Related Depression
- Persistent sadness or hopelessness lasting more than 2 weeks
- Losing interest in activities you previously enjoyed
- Deliberately skipping medicines or blood sugar checks
- Isolating yourself from family and friends
- Feeling that managing diabetes is simply not worth the effort
- Extreme fatigue beyond what diabetes itself causes
💡 Indian Context: In India, mental health struggles are still heavily stigmatised. Many diabetic patients silently suffer from depression for years — telling nobody because of fear of being called “kamzor” — weak. Family members often dismiss emotional struggles saying “sab theek ho jayega” — everything will be fine. This silence is dangerous and costs lives.
What You Can Do
According to 2024 ADA Standards of Care — every diabetic patient should be screened for depression and diabetes distress at least once a year.
Practical steps that genuinely help:
- Talk to your doctor honestly — mention your emotional state, not just blood sugar numbers
- Join a diabetes support group — shared experiences reduce isolation significantly
- Regular exercise — proven to reduce depression symptoms as effectively as mild antidepressants
- Cognitive Behavioural Therapy (CBT) — highly effective for diabetes distress
- Never skip medicines when feeling low — this is when blood sugar control matters most
⚠️ Important: If you or a family member with diabetes is experiencing persistent sadness, hopelessness or thoughts of self-harm — please consult a doctor immediately. Depression is a medical condition. It deserves medical treatment — just like high blood sugar does.
Reference:
The Importance of Addressing Depression and Diabetes Distress in T2D — PMC
Depression, Anxiety and Quality of Life in T2D — PMC 2024
Integrating Mental Health into Diabetes Care — PMC 2024
Prevalence and Predictors of Depression in T2D India — PMC
Now we understand the complications of type 2 diabetes, lets now prepare a strategy to battle these complications.
Acting on that knowledge — at every single doctor visit — is what actually saves lives.
Here is your complete evidence-based checklist based on 2024 ADA Standards of Care:
Every Visit — Every 3 Months ✅
- Check HbA1c — target below 7%
- Check blood pressure — target below 130/80 mmHg
- Review current medications — any side effects?
- Check feet — remove shoes and socks at every visit
- Discuss lifestyle — diet, exercise, sleep, stress
Every Year — Annual Tests ✅
- Urine microalbumin test — kidney early warning
- Dilated eye examination — retinopathy screening
- Lipid profile — cholesterol and triglycerides
- Kidney function test — serum creatinine and eGFR
- ECG — heart screening
- Foot sensation test — monofilament test for neuropathy
- Depression and diabetes distress screening
- Vitamin B12 level — especially if on Metformin
Once — Vaccinations ✅
- Influenza vaccine — every year
- Hepatitis B vaccine — if not previously given
- Pneumococcal vaccine — especially above 65 years
🩺 From My Medical Studies “In our community medicine postings, we learned that most diabetes complications are entirely preventable with systematic monitoring. The tragedy in India is not lack of treatment — it is lack of timely screening. A ₹100 urine microalbumin test can prevent kidney dialysis. A ₹300 eye examination can prevent blindness. The checklist above is not optional — it is the difference between a diabetic patient who lives well and one who doesn’t.” — Mohammad Junaid Rain, MBBS 2nd Year
💡 Indian Tip: Print this checklist. Take it to every doctor appointment. Tick each item. Your doctor will respect your proactiveness — and your organs will thank you for life.
Reference:
ADA Standards of Care in Diabetes 2024
Your Guide to 2024 ADA Standards of Care — DiaTribe
About the author
It’s me Mohammad Junaid Rain an MBBS student at GMC Nagpur, passionate about making evidence-based medical information accessible to every Indian. “medstuffs.com” is dedicated to clear, doctor-written disease education for patients and caregivers.
Disclaimer: This article is for educational purposes only and does not substitute professional medical advice. Please consult your doctor for diagnosis and treatment.